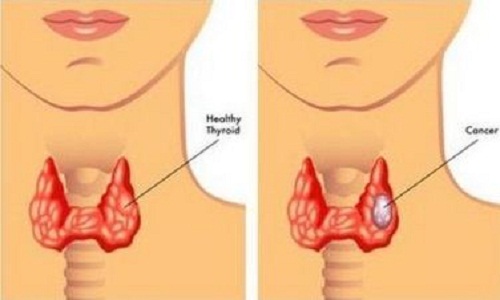
Throat cancer
Throat cancer refers to cancerous tumors that develop in your throat (pharynx), voice box (larynx) or tonsils.
Your throat is a muscular tube that begins behind your nose and ends in your neck. Throat cancer most often begins in the flat cells that line the inside of your throat.
Your voice box sits just below your throat and also is susceptible to throat cancer. The voice box is made of cartilage and contains the vocal cords that vibrate to make sound when you talk.
Throat cancer can also affect the piece of cartilage (epiglottis) that acts as a lid for your windpipe. Tonsil cancer, another form of throat cancer, affects the tonsils, which are located on the back of the throat.
What is throat cancer?
Throat cancer is uncontrolled cell growth in the throat.
The throat has many parts, and most of them can develop cancer. Around 3,000 different cancers start in a part of the pharynx.
Throat cancer is rare compared to other types. According to the National Cancer Institute (NCI), pharyngeal cancers occur in about 1 percent of adults in the U.S., and less than 0.5 percent of adults are likely to have cancer of the larynx.
The survival rate depends on the stage of the cancer and the area affected. 60.7 percent of people with laryngeal cancer survive for longer than 5 years, compared to 64.5 percent of individuals with pharyngeal cancer.
Many types of throat cancer begin as squamous cell carcinoma. This occurs in the squamous cells that line the throat. It is listed by the American Cancer Society (ACS) as a skin cancer but runs the risk of developing into throat cancer when it affects the skin around the throat.
Types of throat cancer
There are several types of throat cancer. Although all throat cancers involve the development and growth of abnormal cells, your doctor has to identify your specific type to determine the most effective treatment plan. The two primary types of throat cancer are:
- Squamous cell carcinoma. This type of throat cancer affects the flat cells lining the throat. It’s the most common throat cancer in the United States.
- Adenocarcinoma. This type of throat cancer affects the glandular cells, and is rare.
Along with these two main types, throat cancer can be broken into two additional types. One type is pharyngeal cancer, which develops in the neck and throat. This includes:
- nasopharynx cancer (upper part of the throat)
- oropharynx cancer (middle part of the throat)
- hypopharynx cancer (bottom part of the throat)
The other type is laryngeal cancer, which affects the larynx or voice box.
Symptoms
Every type of throat cancer is different. Symptoms depend on the stage and location of the cancer.
Common early symptoms of laryngeal and pharyngeal cancer include:
- difficulty swallowing
- voice changes, especially hoarseness or not speaking clearly
- sore throat
- unexplained weight loss
- swelling of the eyes, jaw, throat, or neck
- bleeding in the mouth or nose
- a long-lasting cough
- coughing up blood
- a lump or sore that does not heal
- wheezing or breathing problems
- pain when swallowing
- ear pain
- swollen lymph nodes in the neck
These symptoms can come from less serious conditions, but it is important that a doctor checks them to rule out the presence of a type of throat cancer.
Make a doctor’s appointment if you have any of these symptoms and they do not improve after two to three weeks.
Causes and risk factors
Men are more likely to develop throat cancer than women. Certain lifestyle habits increase the risk of developing cancer of the throat, including:
- smoking
- excessive alcohol consumption
- poor nutrition
- exposure to asbestos
- poor dental hygiene
- genetic syndromes
- Gastroesophageal reflux disease (GERD)
Throat cancer is also associated with certain types of human papillomavirus infections (HPV). HPV is a sexually transmitted virus. HPV infection is a risk factor for certain oropharyngeal cancers, according to the Cancer Treatment Centers of America.
Throat cancer has also been linked to other types of cancers. In fact, some people diagnosed with throat cancer are diagnosed with esophageal, lung, or bladder cancer at the same time. This may be because these cancers have some of the same risk factors.
Prevention
There's no proven way to prevent throat cancer from occurring. But in order to reduce your risk of throat cancer, you can:
- Stop smoking or don't start smoking. If you smoke, quit. If you don't smoke, don't start. Stopping smoking can be very difficult, so get some help. Your doctor can discuss the benefits and risks of the many stop-smoking strategies, such as medications, nicotine replacement products and counseling.
- Drink alcohol only in moderation, if at all. If you choose to drink alcohol, do so in moderation. For healthy adults, that means up to one drink a day for women of all ages and men older than age 65, and up to two drinks a day for men age 65 and younger.
- Choose a healthy diet full of fruits and vegetables. The vitamins and antioxidants in fruits and vegetables may reduce your risk of throat cancer. Eat a variety of colorful fruits and vegetables.
- Protect yourself from HPV. Some throat cancers are thought to be caused by the s*xually transmitted infection human papillomavirus (HPV). You can reduce your risk of HPV by limiting your number of s*xual partners and using a condom every time you have s*x. Also consider the HPV vaccine, which is available to boys, girls, and young women and men.
Diagnosis
In order to diagnose throat cancer, your doctor may recommend:
-
Using a scope to get a closer look at your throat. Your doctor may use a special lighted scope (endoscope) to get a close look at your throat during a procedure called endoscopy. A tiny camera at the end of the endoscope transmits images to a video screen that your doctor watches for signs of abnormalities in your throat.
Another type of scope (laryngoscope) can be inserted in your voice box. It uses a magnifying lens to help your doctor examine your vocal cords. This procedure is called laryngoscopy.
-
Removing a tissue sample for testing. If abnormalities are found during an endoscopy or laryngoscopy, your doctor can pass surgical instruments through the scope to collect a tissue sample (biopsy). The sample is sent to a laboratory for testing. Your doctor may also order a sample of a swollen lymph node using a technique called fine-needle aspiration.
-
Imaging tests. Imaging tests, including X-ray, computerized tomography (CT), magnetic resonance imaging (MRI) and positron emission tomography (PET), may help your doctor determine the extent of your cancer beyond the surface of your throat or voice box.
Staging throat cancer
If your doctor finds cancerous cells in your throat, they will order additional tests to identify the stage, or the extent, of your cancer. The stages range from 0 to 4:
- Stage 0: The tumor is only on the top layer of cells of the affected part of the throat.
- Stage 1: The tumor is less than 2 cm and limited to the part of the throat where it started.
- Stage 2: The tumor is between 2 and 4 cm, or may have grown into a nearby area.
- Stage 3: The tumor is larger than 4 cm or has grown into other structures in the throat or has spread to one lymph node.
- Stage 4: The tumor has spread to the lymph nodes or distant organs.
Imaging tests
Your doctor can use a variety of tests to stage your throat cancer. Imaging tests of the chest, neck, and head can provide a better picture of the disease’s progression. These tests may include the following:
- Magnetic resonance imaging (MRI). This imaging test uses radio waves and strong magnets to create detailed pictures of the inside of your neck. An MRI looks for tumors and can determine whether cancer has spread to other parts of the body. You’ll lie in a narrow tube as the machine creates images. The length of the test varies, but typically doesn’t take longer than one hour.
- Positron emission tomography (PET scan). A PET scan involves injecting a type of radioactive sugar into your blood. The scan creates images of areas of radioactivity in your body. This type of imaging test can be used in cases of advanced cancer.
- Computed tomography (CT scan). This imaging test uses X-rays to create a cross-sectional picture of your body. A CT scan also produces images of soft tissue and organs in the body. This scan helps your doctor determine the size of a tumor. It also helps them determine whether the tumor has spread to different areas, such as the lymph nodes and the lungs.
- Barium swallow. Your doctor may suggest a barium swallow if you’re having difficulties swallowing. You’ll drink a thick liquid to coat your throat and esophagus. This test creates X-ray images of your throat and esophagus.
- Chest X-ray. If your doctor suspects that the cancer has spread to your lungs, you’ll need a chest X-ray to check for abnormalities.
Treatment
Your treatment options are based on many factors, such as the location and stage of your throat cancer, the type of cells involved, your overall health, and your personal preferences. Discuss the benefits and risks of each of your options with your doctor. Together you can determine what treatments will be most appropriate for you.
Radiation therapy
Radiation therapy uses high-energy beams from sources such as X-rays and protons to deliver radiation to the cancer cells, causing them to die.
Radiation therapy can come from a large machine outside your body (external beam radiation), or radiation therapy can come from small radioactive seeds and wires that can be placed inside your body, near your cancer (brachytherapy).
For early-stage throat cancers, radiation therapy may be the only treatment necessary. For more-advanced throat cancers, radiation therapy may be combined with chemotherapy or surgery. In very advanced throat cancers, radiation therapy may be used to reduce signs and symptoms and make you more comfortable.
Surgery
If the tumor in your throat is small, your doctor may surgically remove the tumor. This surgery is done in the hospital while you’re under sedation. Your doctor may recommend one of the following surgical procedures:
- Endoscopic surgery. This procedure uses an endoscope, which is a long thin tube with a light and camera at the end, to pass through surgical instruments or lasers to treat early stage cancers.
- Cordectomy. This procedure removes all or part of your vocal cords.
- Laryngectomy. This procedure removes all or a portion of your voice box, depending on severity of the cancer. Some people can speak normally after surgery, but some people must learn how to speak without a voice box.
- Pharyngectomy. This procedure removes a part of your throat.
- Neck dissection. If throat cancer spreads within the neck, your doctor may remove some of your lymph nodes.
Chemotherapy
Chemotherapy uses drugs to kill cancer cells. Chemotherapy is often used along with radiation therapy in treating throat cancers. Certain chemotherapy drugs make cancer cells more sensitive to radiation therapy. But combining chemotherapy and radiation therapy increases the side effects of both treatments. Discuss with your doctor the side effects you're likely to experience and whether combined treatments will offer benefits that outweigh those effects.
Targeted drug therapy
Targeted drugs treat throat cancer by taking advantage of specific defects in cancer cells that fuel the cells' growth.
Cetuximab (Erbitux) is one targeted therapy approved for treating throat cancer in certain situations. Cetuximab stops the action of a protein that's found in many types of healthy cells, but is more prevalent in certain types of throat cancer cells.
Other targeted drugs are being studied in clinical trials. Targeted drugs can be used in combination with chemotherapy or radiation therapy.
Post-treatment recovery
Some people with throat cancer require therapy after treatment to relearn how to speak. This can be improved by working with a speech therapist and a physical therapist.
In addition, some people with throat cancer experience complications. These may include:
- difficulty swallowing
- disfigurement of the neck or face
- inability to speak
- difficulty breathing
- skin hardening around the neck
You can discuss reconstructive surgery with your doctor if you have face or neck disfigurement after surgery. Occupational therapists can help with swallowing difficulty.
Alternative medicine
No alternative treatments have proved helpful in treating throat cancer. However, some complementary and alternative treatments may help you cope with your diagnosis and with the side effects of throat cancer treatment. Talk to your doctor about your options.
Alternative treatments you may find helpful include:
- Acupuncture
- Massage therapy
- Meditation
- Relaxation techniques
Coping and support
Being diagnosed with cancer can be devastating. Throat cancer affects a part of your body that is vital to everyday activities, such as breathing, eating and talking. In addition to worrying about how these basic activities may be affected, you may also be concerned about your treatments and chances for survival.
Though you may feel like your life — your survival — is out of your hands, you can take steps to feel more in control and to cope with your throat cancer diagnosis. To cope, try to:
- Learn enough about throat cancer to make treatment decisions. Write down a list of questions to ask your doctor at your next appointment. Ask your doctor about further sources of information about your cancer. Knowing more about your specific condition may help you feel more comfortable when making treatment decisions.
- Find someone to talk with. Seek out sources of support that can help you deal with the emotions you're feeling. You may have a close friend or family member who is a good listener. Clergy members and counselors are other options. Consider joining a support group for people with cancer. Contact your local chapter of the American Cancer Society (ACS) or Support for People with Oral and Head and Neck Cancer. The ACS's Cancer Survivors Network offers online message boards and chatrooms that you can use to connect with others with throat cancer.
- Take care of yourself during cancer treatment. Make keeping your body healthy during treatment a priority. Avoid extra stress. Get enough sleep each night so that you wake feeling rested. Take a walk or find time to exercise when you feel up to it. Make time for relaxing, such as listening to music or reading a book.
-
Go to all of your follow-up appointments. Your doctor will schedule follow-up exams every few months during the first two years after treatment, and then less frequently after that. These exams allow your doctor to monitor your recovery and check for a cancer recurrence.
Follow-up exams can make you nervous, since they may remind you of your initial diagnosis and treatment. You may fear that your cancer has come back. Expect some anxiety around the time of each follow-up appointment. Plan ahead by finding relaxing activities that can help redirect your mind away from your fears.